Overview
What is Severe Asthma?
Around 3 to 10% of people with asthma have severe asthma. People with severe asthma require high-dose medications to adequately control their condition. Some still struggle with their asthma symptoms and attacks despite these high-dose medications. It is not exactly clear why certain patients develop severe asthma condition.
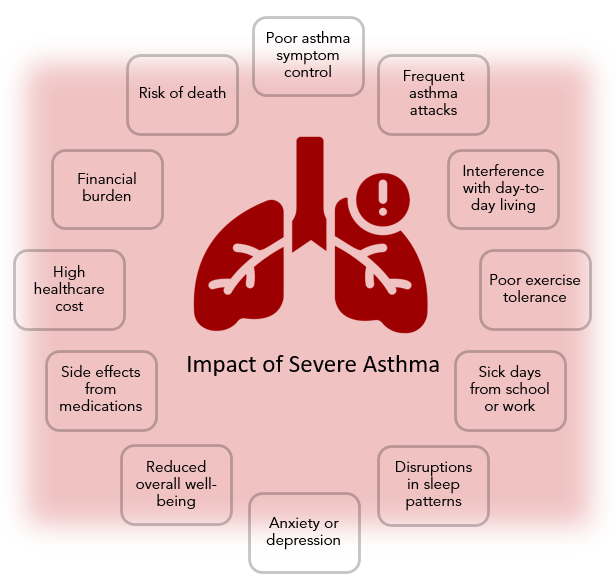
Causes
Diagnosis of Severe Asthma
It is often a long and tedious journey to confirm the diagnosis of severe asthma. It requires a comprehensive evaluation by a Respiratory Physician or Severe Asthma Specialist. Your doctor will go through your medical history in detail and conduct a physical examination. Further tests will be suggested to confirm the severe asthma diagnosis, the type of severe asthma and other contributory conditions.
Types of Severe Asthma
There are many possible root causes and different types of severe asthma. There is still ongoing research to further understand these severe asthma types.
Some of the most common severe asthma types are:
- Allergic (caused by allergens)
- Eosinophilic (associated with an increased level of Eosinophils, which is a type of white blood cells)
- Non-eosinophilic (associated with an increased level of other white blood cells)
Identifying the specific characteristics of these severe asthma types can help to personalise the treatment approach for each individual patient.
Detection & Treatment
Common Tests for Severe Asthma
-
Spirometry
This is a common lung function test that can help to confirm the diagnosis of asthma. It also examines the severity of the airway reactivity or obstruction. You may be asked to withhold your inhalers for several hours to days prior to this test. Depending on your condition, you may need to repeat this test.
-
Fractional Exhaled Nitric Oxide
This lung function test assesses the degree of eosinophilic airway inflammation commonly seen in severe asthma.
-
Allergy Testing
This is usually performed via a skin prick test. It can help to identify your allergic triggers. You should avoid taking anti-histamines, certain anti-depressants and heartburn medications at least one week before this test, as these can interfere with the result. If you are not suitable for a skin prick test, your doctor may order a blood test instead.
-
Blood Tests
A full blood count is usually performed to look at your white blood cells (eosinophil), which is often raised in severe asthma. Other blood tests related to your condition and high-dose medications may also be performed.
-
Sputum Testing
Respiratory infections and inflammation are common in severe asthma. Your phlegm may be collected to look for the presence of infection and inflammation.
-
Chest Imaging
This may be required to identify other causes of your respiratory symptoms. It can be a simple chest X-ray or a more comprehensive Computed Tomography (CT) scan of the chest.
Treatment of Severe Asthma
There is no standard treatment for severe asthma. Your doctor will first try to address the factors contributing to the severity of your asthma. The treatment will need to be adjusted and personalised to each individual over time. Depending on the type of your severe asthma, targeted treatment may also be recommended.
Factors that can be addressed by your doctor:
- Insufficient inhaler dosage
- Failure to take medications as directed
- Incorrect inhaler technique
- Cigarette smoking
- Persistent exposure to triggers or allergens
- Triggers by medications like beta blockers and nonsteroidal anti-inflammatory drugs
- Regular or overuse of reliever (salbutamol inhaler)
- Side effects from asthma medications
- Other medical conditions like gastric reflux, chronic rhinosinusitis, anxiety, depression, heart diseases, obesity, obstructive sleep apnea
1. Maintenance Treatment (Long-term)
Inhaled Corticosteroids
-
These steroid-containing inhalers are the maintenance treatment for severe asthma. These help to:
> Treat the underlying airway inflammation in asthma
> Control asthma symptoms
> Reduce the risk of lung function deterioration and asthma attacks
> Reduce the risk of dying from asthma
Inhaled Long-Acting Beta Agonists (Add-on)
-
These are always prescribed to be used in combination with inhaled corticosteroids in a single combination inhaler device. These help to:
> Relax the muscles around your airways to help keep them open for a longer duration
> Improve your asthma symptoms and reduce the severity of flare-ups
Inhaled Long-Acting Muscarinic Antagonists (Add-on)
-
These inhalers do not contain steroids. These help to:
> Provide additional effect in opening up your airways for a longer duration of time, and may help to reduce asthma attacks
-
These are usually prescribed as:
> A separate inhaler to be used together with your maintenance inhaler, or
> Together with inhaled corticosteroid and long-acting beta agonist in a triple combination inhaler device
2. Reliever Treatment (Short-term/Fast-acting)
Inhaled Short-Acting Beta Agonist (Salbutamol)
- Salbutamol opens up your airway rapidly and is used only for quick relief of your asthma symptoms as needed. Using salbutamol alone or overusing salbutamol puts you at risk of serious asthma attacks and dying from asthma. Remember to use your maintenance inhalers regularly for long term asthma control.
Inhaled Corticosteroid with Formoterol
- For patients who are on maintenance inhaled corticosteroid with formoterol (long-acting beta agonist), you can take one to two additional doses of the same inhaler as needed for quick relief of your asthma symptoms, up to the maximum dosage allowed (as determined by your doctor).
Be familiar with your inhaler device and technique. Incorrect inhaler technique can increase your risk of asthma attacks. If you are unsure of how to use your inhaler, please consult your doctor, nurse or pharmacist for support or scan the following QR code for our patient educational videos available in four different languages.

These videos were produced by Singapore National Asthma Programme and have been reviewed by the Pharmaceutical Society of Singapore and National Medical Information Workgroup.
3. Oral Medications (Add-on)
Montelukast (Leukotriene Antagonists)
- This blocks substances in the body called leukotrienes to help improve symptoms of asthma and allergic rhinitis.
- It is used as add-on therapy for asthmatic patients with allergic rhinitis.
- There is a small risk of neuropsychiatric side effects such as sleep disturbances, suicidality, mood and behavioural changes. Your doctor should discuss the benefits and risks of taking this medication for your asthma.
Azithromycin
- This is an antibiotic that is an emerging add-on therapy in severe asthma due to its anti-inflammatory properties.
- It is usually taken three times a week and is generally well tolerated. It may help to reduce asthma attacks in the long term as deemed appropriate by your doctor.
Prednisolone (Steroid Therapy)
- This is usually reserved as the last treatment option in severe asthma, i.e. if your severe asthma is still poorly controlled despite the use of high-dose inhalers, other add-on therapies including biologics and treatment of contributory factors.
- It is associated with significant side effects such as weight gain, high blood pressure, high sugar, increased chance of infections and osteoporosis.
4. Biologic Therapies
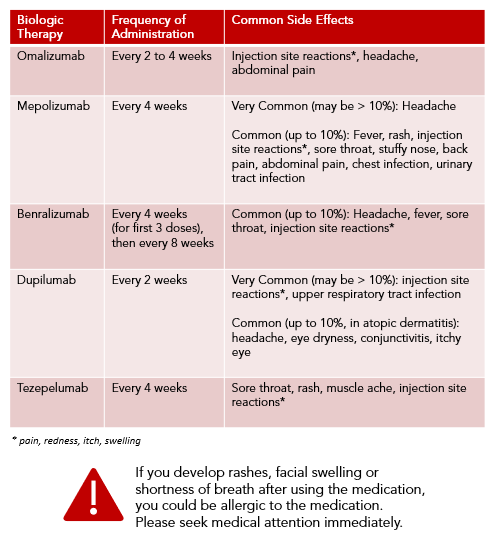
Biologic therapies are treatment for severe asthma that have emerged over the last decade. These are man-made antibodies that target specific cells involved in the inflammation pathways causing your asthma symptoms. There are currently five biologic therapies approved for use in Singapore to treat severe asthma:
- Omalizumab
- Mepolizumab
- Benralizumab
- Dupilumab
- Tezepelumab
Your doctor will advise on the choice of biologic therapy best suited for your severe asthma condition. As these therapies are expensive, please check with your doctor the cost and available funding before embarking on such treatment. They are given as subcutaneous injections (under the skin) in the clinic. These can also be administered at home by the patient or caregiver after they attend a training session.
Care Management
Living with Severe Asthma
You can still lead a normal and healthy lifestyle even if you have severe asthma.

Specialties & Services

