Overview
Incontinence-associated dermatitis (IAD) is a common skin injury caused by prolonged skin contact with urine and/or faeces, experienced by people with incontinence.
You may know it as diaper dermatitis, diaper rash, perineal rash, or perineal excoriation. Good skin care keeps your skin healthy and helps you avoid IAD and its negative consequences.
Causes
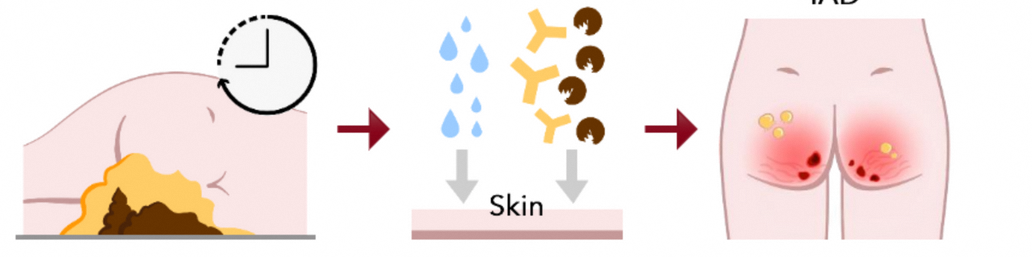
Incontinence happens when there is uncontrollable leakage of urine and/or faeces. There can be many causes of incontinence, like damage to the bladder and bowel structures or brain injury. It causes your skin to be exposed to incontinence waste for a prolonged period of time.
After prolonged contact with incontinence waste, water and substances from urine and/or faeces enter your skin, causing it to swell and become less acidic. In addition, faecal enzymes (proteins in faeces) digest the skin directly. This damages your healthy skin functions and leads to Incontinence-Associated Dermatitis (IAD).
Risk Factors:
- Incontinence of urine and/or faeces.
- Diarrhoea
- Incorrect use of skin or incontinence products.
- Poor skin condition (eg: due to old age, steroid use, diabetes, fragile, dry skin). Poor hygiene.
- Poor nutrition.
- Immobility Impaired sensation. Previous pressure injury.
- Medications (eg: antibiotics, steroids)

Where Does Incontinence-Associated Dermatitis Occur:
IAD can occur wherever your skin comes into contact with urine and/or faeces.
It may also extend to the surrounding skin and skin folds.
Commonly affected areas are:
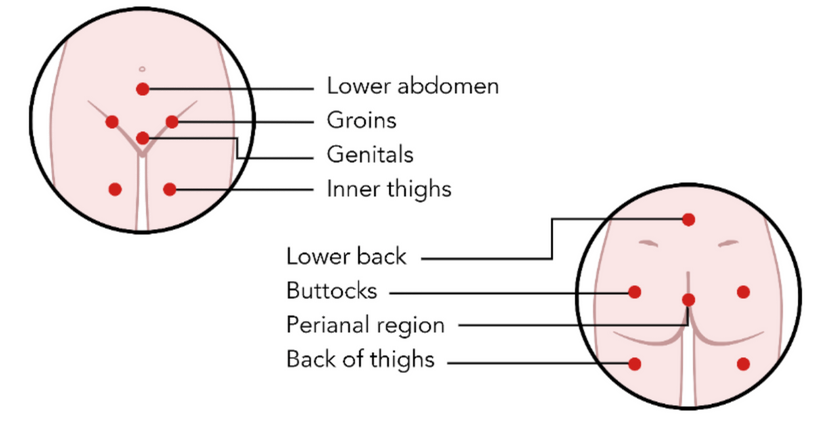
Signs & Symptoms:
For persons with darker skin tones, skin redness may look paler, darker, purplish or yellowish.
You may notice some of these signs and symptoms on areas affected by IAD:
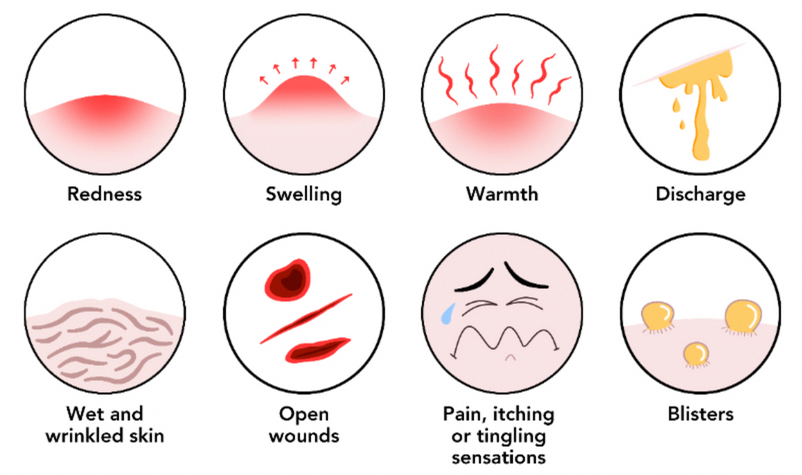
IAD wounds are also prone to skin infections, which may produce the following warning signs:
- White scaly or flaky skin.
- Satellite lesions (small wound(s) near a larger wound).
- Yellow/brown/greyish/greenish discharge. Increase in discharge amount. Shiny appearance.
Consequences if left untreated:
- Pain Disturbed sleep.
- Immobility
- Skin infection.
- Development of pressure injury.
- Reduced quality of life.
- Urinary tract infection.

Prevention
How do I Prevent or Manage Incontinence-Associated Dermatitis?
You can use the same steps for both IAD prevention and management.
Use the acronym A-C-P-R-O to guide you along. You can discuss with your doctor or nurse to learn more.
Care Management
A – Assess

Check for IAD at all skin at risk of, or in contact with urine and/or faeces (eg: genitals, groins, buttocks and nearby skin folds).
Check skin condition:
- Daily
- When changing incontinence aids.
- When cleansing the skin.
C – Cleanse
Use skin cleansers that are specially formulated for incontinence cleansing.
- "No-rinse" reduces skin trauma from repeated washing and drying.
- "pH-balanced" preserves your skin's natural acidity, which is important for maintaining healthy skin.
- Soft non-woven disposable wipes reduce skin trauma and improve hygiene.
- Avoid cleaning with regular soap often depletes skin acidity, while using water alone can cause swelling, worsening IAD.
- Avoid using non prescribed oil based cream or lotion.
- Cleanse your skin gently at least once per day, and after every episode of incontinence.



- For females: Clean from front to back in one direction, avoid cleaning back and forth to prevent urinary tract infection.
- For males: Retract foreskin (if uncircumcised) and clean from the tip of the penis to the back in one direction, avoid cleaning back and forth to prevent urinary tract infection.
- Dab dry the skin thoroughly after cleaning.
P – Protect
- Apply a thin layer of skin protectant over all skin at risk of contact with urine and/or faeces after cleansing. Skin protectants are products which form a barrier between your skin and incontinence waste to prevent IAD. This barrier prevents further injury and allows the skin beneath it to recover.
- Use sliding sheet when positioning to prevent friction and shear.
- Regular repositioning to relieve pressure and allow ventilation of the skin.
- Manage incontinence to reduce your skin's contact with urine and/or faeces, lowering your risk of developing IAD.
- Speak to your healthcare provider about relieving incontinence or reducing skin contact with incontinence waste. Some ways may include medication changes, bladder or bowel training, and the use of urinary or faecal catheters.
R – Restore
- Apply moisturisers only as directed by your healthcare provider.
- Most skin cleansers and protectants already contain moisturisers. Extra moisturisation may not be required.

O – Observe
Consult your healthcare provider if you observe the following:
- No improvement in IAD after 3 to 5 days of treatment.
- Worsening of IAD (eg: increase in skin redness, pain, wounds).
- Signs of infection at IAD area.
- Persistent rashes at the perineal/groin area to exclude fungal infections.
Your healthcare provider may adjust the course of treatment or refer you to a specialist for further follow-up.

Specialties & Services

