Overview
Fecal incontinence, also known as a bowel incontinence, is the inability to control bowel movements causing stool (feces) to leak unexpectedly from the rectum. Fecal incontinence may include the following:
- Flatus (gas).
- Liquid stool elements and mucus.
- Solid faeces.
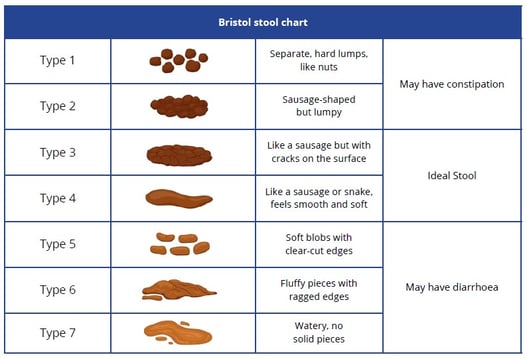
Please refer to the Bristol stool chart and observe the kind of stools you have.
Causes
While it is normal to have more than one cause for fecal incontinence, it is also not unusual for fecal incontinence to happen without a clear cause.
There are many potential causes of fecal incontinence, including:
- Muscle weakness or damage.
- Nerve damage due to diabetes, spinal cord injury or other conditions.
- Severe constipation may cause impacted stools.
- Diarrhoea due to an infection or irritable bowel syndrome.
- Loss of storage capacity in the rectum.
- Rectal prolapse – a condition that causes the rectum to drop out through the anus that stopping the muscles around your anus to close completely.
- Rectocele (for female) – a condition that causes your rectum to bulge through your vagina.
- Using laxatives over a long period of time.
Most incidents of fecal incontinence usually happen when you are having episodes of severe diarrhoea. Some people may have recurring or chronic fecal incontinence that can involve frequent or occasional accidental leakage.
There are two types of fecal incontinence:
- Urge incontinence - When you experience a sudden and strong need to defecate and you are not able to make it to the bathroom in time.
- Passive incontinence - When you are not aware of the need to defecate.
Fecal incontinence may also be accompanied by other bowel problems, such as:
- Diarrhoea
- Constipation
- Gas and bloating.
- Abdominal pain or cramping.
- Irritated or itchy anus.
Care Management
Procedures/ Nursing Interventions:
1. Do pelvic floor exercises

The pelvic floor muscles are layers of muscles stretched like a hammock from the pubic bone at the front of the bottom of the backbone.
The pelvic floor muscles, if weakened, cannot support the openings effectively.
Pelvic floor exercises help strengthen the pelvic floor muscles, which support the bladder, bowel and in women, the uterus and improve bowel control.
Seek advice from your healthcare professional before doing these exercises to make sure you are doing them properly.
They may also be able to suggest additional exercises, exercise devices or muscle stimulation which could speed up the process.
2. Making changes to your diet
What you eat and drink affects the consistency of your stool. You may be able to gain better control of your bowel movements by:
- Keeping track of what you eat. Make a list of what you eat for a week. You may discover a connection between certain foods and your bouts of incontinence. Once you have identified foods that affects your bowel, stop eating them and see if your incontinence improves.
Food that may worsen fecal incontinence:
- Spicy food.
- Fatty and greasy food.
- Cured or smoked meat.
- Carbonated beverages.
- Daily products (if you are lactose intolerant).
- Food that have the same effect as laxatives such as caffeine-containing drinks and alcohol, sugar-free gum and soda.
- Eat smaller meals. Eating three main meals a day may stimulate your bowel to move faster. Instead, eat small frequent meals throughout the day.
- Getting adequate fibre. Fibre helps to make your stool soft and easier to control. Fibre can be found in fruits, vegetables and whole-grain breads and cereals. You should have at least 20 to 30 grams of fibre daily, but avoid adding it to your diet suddenly or all at once as this may cause bloating and gas.
- Drinking more water. Water helps to keep your stools soft and formed. You should drink at least 8 glasses of water daily.
3. Taking care of your skin
You can help avoid discomfort from fecal incontinence by keeping the skin around your anus as clean and dry as possible. This will help relieve anal discomfort and prevent any possible odor associated with fecal incontinence:
- Gently wash the area with water after each bowel movement. Soap or rubbing with dry toilet paper can dry and irritate the skin. Pre-moistened, alcohol-free, perfume-free wipes may be good alternative for cleaning the area.
- Dry thoroughly. Allow the area to air-dry, if possible. If you are short on time, you can gently pat the area dry with toilet paper or washcloth.
- A moisture-barrier cream on the clean and dry area will help keep irritated skin from having direct contact with feces. Non-medicated talcum powder or cornstarch also may help relieve anal discomfort.
- Wear cotton underwear and loose clothing. Tight clothing can restrict airflow, making skin problems worse. Be sure to change soiled underwear quickly.
Specialties & Services

