Overview
What is Dysphagia?
Dysphagia is a swallowing disorder. Patients with a swallowing disorder may face the risk of developing pneumonia (chest infection), whereby food/fluid enter the lungs.
In general, there are 3 swallowing stages:
In the Mouth (Oral Stage)
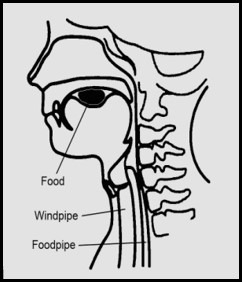
Food is chewed into a bolus (ball) and pushed to the back of the mouth by the tongue to trigger a swallow.
In the Throat (Pharyngeal Stage)
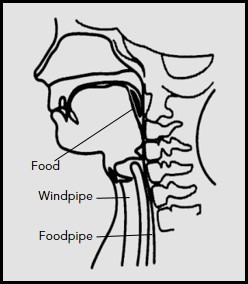
The throat is separated into 2 openings at the lower end: the trachea/airway (below the voice box) and the oesophagus/foodpipe. When the food is pushed to enter the foodpipe, a flap-like structure called the epiglottis, covers the airway to prevent any leakage into the lungs.
In the Foodpipe (Oesophageal Stage)
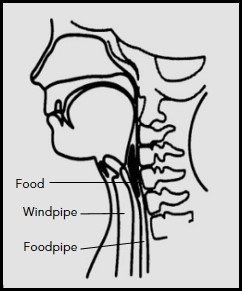
At this stage of swallowing, the airway is sealed and the sphincter (valve) at the top of the foodpipe opens up to allow the food/fluid to slide down with muscular action.
Subsequently, the sphincter at the end of the foodpipe opens up to allow the bolus to enter the stomach.
Causes
- After-effects of a surgery that involves the removal of lumps or tumours in the mouth, throat or foodpipe
- Side effects from chemotherapy or radiotherapy
- Neurological issues such as stroke, head injury, Parkinson's, etc
- Respiratory (breathing) problems
- Multiple medical conditions that weaken the swallowing system
- Ageing
- Difficulty in swallowing saliva or drooling
- Presence of residue of food/fluid in the mouth after swallowing
- Chewing/sucking difficulties
- Wet voice or throat noises after swallowing
- Throat-clearing, choking or coughing during or after swallowing
- Shortness of breath after swallowing
- Recurrent chest infection or fever
- Unintended/ unexplained weight loss
Detection & Treatment
Diagnosis
Your doctor will review your symptoms and may refer you to a Speech Therapist for an assessment of your swallowing status. The therapist will then do a physical examination and assess your swallowing when you eat or drink.
Further instrumental examination may be required e.g. doing a video X-ray (Videofluoroscopy) or a scope (Flexible Endoscopic Examination of Swallowing) when deemed necessary.
Care Management
How is Dysphagia Managed?
Patients with dysphagia are co-managed by the doctor and the speech therapist. Management of your swallowing condition may include:
- Modification to the type, texture and consistencies of your food or fluid
- Oral-motor exercises
- Specific swallowing strategies for safe swallowing
- Use of instrumental devices e.g. surface electro-myographic feedback, a nose scope, special cutlery to assess and/or teach therapy techniques
Tips to Improve Your Swallowing
- Keep upright when eating/drinking
- Take small sips when drinking. Using a straw to suck may be difficult to control the rate and amount of fluid intake, causing you to cough
- Take small, bite-sized mouthfuls when eating
- Do not drink more water to flush food down when you cough while eating/ drinking. Cough out any food/ fluid first and let your breathing settle before you continue to eat or drink
- Take soft foods such as porridge, bean curd and oats
- Chop up fibrous/ hard foods e.g. vegetables, fruits and meat
- Separate the solids from the liquids e.g. do not put noodles in a spoon of soup to eat. Try to swallow the noodles completely before drinking the soup
- Use thickening agents to hold food together e.g. corn flour, sauces, gravy or fluid thickener to allow easier swallowing
- Avoid talking with food in your mouth. Cut down distractions during eating/drinking
If your condition persists or worsens, please consult your doctor or speech therapist.
Specialties & Services

