Overview
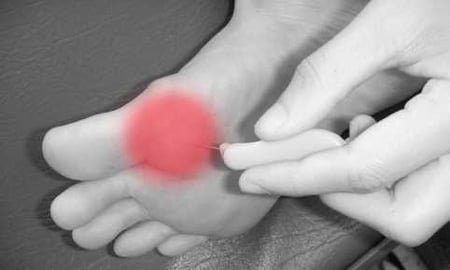
Neuropathy (nerve damage) is a common complication of poorly-controlled diabetes.
People with diabetes neuropathy may experience numbness or loss of protective sensation. They may not feel pain associated with trauma, injury or temperature changes to the same level as those people without neuropathy. This can result in foot injuries going unnoticed, which can develop into serious foot ulcers.
They may also experience tingling, burning, sharp or cramping pain over their feet affecting their quality of life. For some individuals, they may have extreme sensitivity to touch such that light touch from blankets may be painful.
Neuropathy may also lead to changes in bones, muscles, and joints of the feet. Over time, with nerves being affected, one may not notice a change in foot structure or not feel pain with continued weightbearing on the injured foot resulting in a change in foot shape.
What are the risk factors?
The risk of diabetic neuropathy is higher with a longer duration of diabetes, especially poorly controlled diabetes. Other risk factors includes:
- Age
- Alcohol consumption can worsen diabetes neuropathy
- Being overweight
- Diabetes Kidney Disease
- High cholesterol
- Hypertension
- Long duration of diabetes
- Poorly controlled diabetes
- Smoking
What are the potential complications?
- Loss of Limb
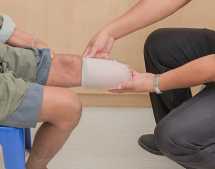
- Charcot Foot
Peripheral neuropathy is the most common type of diabetes neuropathy. If you have any of the following symptoms, you may share with your doctor or healthcare team during your next clinic consultation or foot checks.
1. Feeling Pain
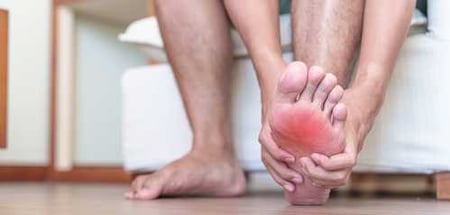
- I feel "pins and needles" or tingling sensation in my feet
- I have burning, stabbing, shooting pain in my feet, especially at night
- My skin over my feet or legs are very sensitive to touch such that I have pain when the blanket touches my feet.
2. Feeling Numbness

- I am not able to feel my feet and I feel unsteady like walking or standing on cotton wool.
- I cannot feel a lot of pain or any pain when my toe is accidentally cut or pierced by a sharp object, or burnt by hot surface.
- My feet are numb and feels like there is a layer of dead skin over it.
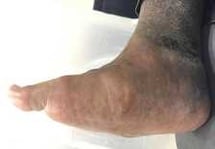
3. Changes in Foot Shape
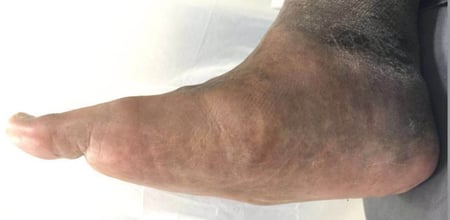
- I noticed that my foot shape has change.
4. Open wounds (Diabetes foot ulcers)
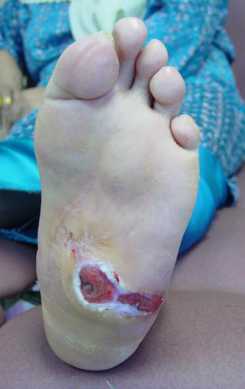
- I have foot ulcer(s) on the bottom of my feet with thickened skin and they take a long time to heal.
Detection & Treatment
What are the screening tests?
- Monofilament testing
- Tuning fork vibration testing 1
- Neurothesiometer testing
1 Source: Al-Muzaini, A., & Baker, N. R. (2017). User's guide to diabetic foot screening [Photograph]. The Diabetic Foot Journal Middle East Vol 3 No 2 2017.
When should I seek medical treatment?
You are advised to seek medical treatment when you have foot ulcer, foot shape changes, or worsening pain over your foot.
Care Management
What can I do?
- Go for your foot screening at least once annually
- Get your diabetes, high blood pressure, and high choloesterol under control
- Care for the feet to prevent complications including daily inspection of feet and footwear
- Take medicine to reduce pain
- Take your medication for diabetes as prescribed
Specialties & Services

